Pimples and acne before a period are common hormonal skin changes experienced by many women during the menstrual cycle. These breakouts occur when hormonal fluctuations increase oil production and clog pores, especially in the days before menstruation.
Pimples can also appear as hormone levels rapidly shift. Understanding how estrogen, progesterone, and androgen levels affect your skin explains why monthly acne happens and how you can prevent hormonal breakouts naturally with skincare, lifestyle changes, and cycle tracking.
What are pimples before the period?
Period pimples are a type of hormonal acne that appears around the time of your menstrual cycle. Unlike bacterial breakouts or hygiene issues, these are caused by changes in your hormones.
Hormonal acne basics
Hormonal pimples usually appear at the same time each month. Your skin reacts to changes in hormones like estrogen and progesterone, which rise and fall during your cycle.
Why cycles affect skin
Throughout your 28-day (average) cycle, your skin changes. One week, it may be dry and glowing. Next, it may be oily and prone to period pimples on the face, depending on which hormone is dominant.
Why do pimples happen before the period?
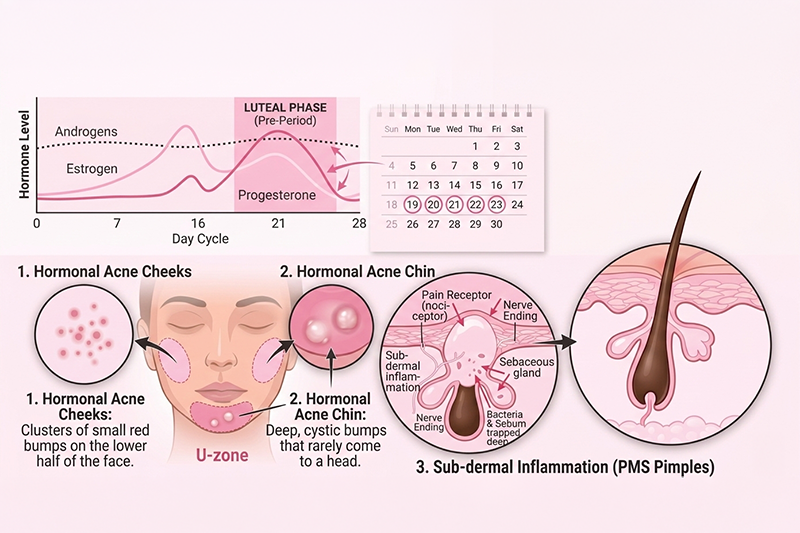
Hormonal changes before menstruation
In the last week of your cycle, usually from day 21 to 28, your body enters the luteal phase and gets ready for your period. If you are not pregnant, estrogen and progesterone levels drop quickly. This change makes your skin react differently.
Progesterone and testosterone increase
Progesterone peaks in the middle of the luteal phase and can cause your pores to swell shut. Just before your period, progesterone drops. Meanwhile, “male” hormones called androgens (like testosterone) remain steady. When estrogen drops, these androgens have a greater impact on your sebaceous glands.
Increased oil production
The spike in androgens is the main reason for acne before your period. Androgens signal your skin to make more sebum (oil). This extra oil can trap dead skin cells and bacteria in your pores.
Pimples during periods – Is it normal?
Yes, experiencing acne during your period is normal. In fact, research suggests that about 63% of women who are prone to acne notice their breakouts get worse during their period.
- Hormone drop explanation: As you begin bleeding, your hormones are at their lowest point, which can leave your skin sensitive and depleted.
- Inflammation response: Prostaglandins (chemicals that cause uterine cramps) can also increase inflammation in your body. This can make period acne look redder and feel more painful.
- Skin sensitivity: Your skin is more easily irritated during your period, so products that normally work may cause redness.
Hormone timeline: How your menstrual cycle affects acne
Understanding the phases of your cycle helps you predict when hormonal pimples will appear.
| Cycle phase | Hormone activity | Skin condition |
| Follicular phase (CD 6 – 13) | Estrogen rises | Skin looks hydrated and clear |
| Ovulation phase (CD 14) (approx.) | LH and estrogen peak | The “glow” phase, though some may feel oily |
| Luteal phase (CD 15 – 28) | Progesterone peaks then drops | High oil production; acne before the period starts |
| Menstrual phase (CD 1 – 5) | All hormones are low | Skin is dry, sensitive, and healing from breakouts |
Note: Some women also experience pimples during ovulation due to the sudden rise in Luteinising Hormone (LH).
Acne before period or pregnancy – How to tell the difference?
Since both involve high progesterone levels, it can be tricky to tell them apart.
- Period pimples usually subside once your period begins. If your skin stays broken out and your period is late, it could be related to pregnancy.
- Pregnancy acne often comes with strong breast tenderness and morning sickness. PMS pimples usually happen with bloating and irritability.
Common symptoms of hormonal acne before the period

If you aren’t sure your breakouts are cycle-related, look for these signs:
- Hormonal acne chin: Deep, cystic bumps that rarely come to a head
- Hormonal acne cheeks: Clusters of small red bumps on the lower half of the face
- PMS pimples: Breakouts that are often “blind” (painful bumps under the skin)
Where do period pimples usually appear?
Hormonal receptors are most common in the lower third of your face. Period acne most commonly appears on:
- chin
- jawline
- lower cheeks
What hormones cause acne in women?
- Estrogen: Generally, the “skin-friendly” hormone that keeps skin plump and clear.
- Progesterone: Increases sebum production and can cause skin swelling that traps oil.
- Androgens: The primary drivers of hormonal pimples; they stimulate oil glands to go into overdrive.
How to naturally prevent acne before your period
Lifestyle fixes
Prioritise 7–9 hours of sleep. Lack of sleep increases cortisol levels, which triggers more oil production.
Diet adjustments
Lower your sugar and dairy intake the week before your period. High-glycemic foods spike insulin levels, which worsens acne before your period.
Skincare routine
Switch to a gentle, non-comedogenic cleanser. Avoid heavy oils and use water-based moisturisers.
Stress reduction
Stress creates cortisol. Practice yoga or deep breathing during your luteal phase to help keep your hormones balanced.
How to stop hormonal acne fast (dermatologist tips)
If natural methods are not working, consider these targeted treatments:
- Retinoids: Help increase cell turnover so pores don’t clog
- Salicylic acid: A BHA that dissolves the oil, causing period pimples
- Zinc: An oral supplement or topical ingredient that reduces inflammation
- Medical treatments: For severe cases, doctors may prescribe birth control or spironolactone to regulate androgens
Note: Use only with a dermatologist’s advice. It is essential to consult with a healthcare professional or dermatologist before starting these treatments to ensure they are safe and appropriate for your specific skin needs.
Pimples during ovulation – Why breakouts also happen mid-cycle
Most people focus on period breakouts, but pimples can also happen during ovulation. Around day 14, a spike in estrogen and LH can make your skin oily and cause ‘ovulation acne’ for some women.
When should you see a doctor?
If your hormonal pimples are leaving scars, causing emotional distress, or are accompanied by irregular periods and excess hair growth (potential signs of PCOS), consult a dermatologist or gynecologist.
Track your cycle to predict acne breakouts
The best way to manage your skin is to stop being surprised by it. Using a tool like the Premom app, you can track ovulation and predict your cycle. When you know your luteal phase begins, you can start using salicylic acid or reducing sugar before the first pimple appears.
If you are unsure how to manage your period acne, you can connect with our experts through the Ask an Expert (AAE) feature inside the Premom app. We are here to help you through your cycle with evidence-based guidance.
FAQ‘s – About Acne pimples before period
It all comes down to a “hormonally perfect storm” occurring in your body about 7–10 days before bleeding begins. After ovulation, your estrogen levels drop. Estrogen is generally “skin-friendly” because it keeps oil production low.
As it dips, androgens (like testosterone) become more dominant. These androgens stimulate your sebaceous glands to produce excess sebum (oil). When this thick oil mixes with dead skin cells, it clogs your pores, leading to acne before your period.
The easiest way to tell is by looking at the pattern and location.
Hormonal acne: Usually appears like clockwork once a month. It is concentrated on the “U-zone” (chin, jawline, and neck) and often manifests as deep, painful cysts that don’t always come to the head.
Bacterial/Surface acne: This can appear anywhere on the face (forehead, nose, or cheeks) and is often caused by external factors like sweat, dirty pillowcases, or makeup. It usually looks like small whiteheads or blackheads that respond quickly to topical treatment.
While you can’t stop your hormones from shifting, you can change how your skin reacts to them. The key is proactive skincare. About a week before your period is due, start using a chemical exfoliant, such as salicylic acid.
This oil-soluble acid penetrates deep into pores to clear out excess sebum before it can form a blockage. Reducing high-glycemic foods (sugar and white bread) this week also helps keep insulin levels stable, which reduces androgen activity.
If a breakout has already surfaced, the goal is to reduce inflammation.
Spot Treatments: Use Benzoyl Peroxide to kill bacteria or Salicylic acid to unclog the pore. These should be used only on medical advice.
Don’t Pop: Period pimples are often “blind” (deep under the skin). Squeezing them won’t push the oil out; it will only push the infection deeper, leading to scarring and longer healing times.
Ice: If a cyst is particularly painful, apply a clean ice pack for 5 minutes to constrict blood vessels and reduce swelling.
Period acne typically occurs in the lower third of the face. Specifically, the chin, jawline, and sides of the neck. This area has a higher density of oil glands, which are particularly sensitive to increases in androgens and decreases in estrogen.
The Luteal Phase (CD 15 – 28) is the primary culprit. This is the stage between ovulation and the start of your period. During the late luteal phase, progesterone peaks and then crashes along with estrogen. This fluctuation causes the skin to swell and pores to compress, trapping oil inside.
This is why you likely notice pimples around 3–7 days before your period starts, on day 1 of your cycle.
Natural prevention focuses on internal balance:
Diet: Focus on anti-inflammatory foods like wild-caught fish (Omega-3s), leafy greens, and Zinc-rich seeds.
Stress management: High cortisol levels (the stress hormone) directly worsen hormonal pimples.
Supplements: Many women find relief using Vitex (Chasteberry) or Magnesium, though you should consult a doctor before starting new supplements to ensure they don’t interfere with your specific hormone levels.
This is a common point of confusion because both involve high progesterone levels.
Period: If PMS symptoms like cramping and then disappear once your flow starts, it’s cycle-related.
Pregnancy: If the acne is persistent, your period is late, and you are experiencing unusual fatigue or breast tenderness, it could be pregnancy. During pregnancy, a massive surge in hormones can cause “glow” for some, but intense breakouts for others.
Unlike a standard whitehead, period acne often looks like red, angry, and inflamed bumps. They are frequently “sub-dermal,” meaning they sit under the skin and feel sore to the touch. Because they are driven by internal hormones rather than surface dirt, they often take longer to “heal” and disappear than a typical blemish.
For most women, it starts 3 to 10 days before their period begins. This is when the hormone shift is most dramatic.
Usually, these breakouts begin to clear up within 3 to 5 days after your period starts. As your estrogen levels begin to climb again during the new follicular phase, your skin’s oil production stabilises, and the inflammation subsides.
If your hormonal pimples on the chin are accompanied by irregular periods or excess hair growth, it could be PCOS (Polycystic Ovary Syndrome). PCOS pimples are often more severe, cover a larger area of the jaw and neck, and rarely go away entirely, even after your period ends.
Disclaimer: This content is for educational purposes only and is not medical advice. Please consult a healthcare professional for personalised guidance.
References
- Amuzescu A, Tampa M, Matei C, Georgescu SR. Adult female acne: recent advances in pathophysiology and therapeutic approaches. Cosmetics. 2024;11(3):74. doi:10.3390/cosmetics11030074, https://www.mdpi.com/2079-9284/11/3/74
- Lakshmi C. Hormone therapy in acne. Indian J Dermatol Venereol Leprol. 2013;79(3):322. doi:10.4103/0378-6323.110765, https://pubmed.ncbi.nlm.nih.gov/23619437/
- Ghosh S, Chaudhuri S, Jain V, Aggarwal K. Profiling and hormonal therapy for acne in women. Indian J Dermatol. 2014;59(2):107. doi:10.4103/0019-5154.127667, https://pubmed.ncbi.nlm.nih.gov/24700926/
- Bagatin E, Freitas THP, Rivitti-Machado MC, et al. Adult female acne: a guide to clinical practice. An Bras Dermatol. 2019;94(1):62-75. doi:10.1590/abd1806-4841.20198203, https://pubmed.ncbi.nlm.nih.gov/30726466/
- Khunger N, Kumar C. A clinico-epidemiological study of adult acne: is it different from adolescent acne? Indian J Dermatol Venereol Leprol. 2012;78(3):335. doi:10.4103/0378-6323.95450, https://pubmed.ncbi.nlm.nih.gov/22565434/
- Nguyen ML, Nguyen S, Sood N, Marivada S, Magaldino A, Mayrovitz HN. Physiological changes in women’s skin during the menstrual cycle: a scoping review. Cureus. 2024;16(12):e75286. doi:10.7759/cureus.75286, https://pubmed.ncbi.nlm.nih.gov/39776723/
- Smith CA, Gosnell E, Karatas TB, et al. Hormonal therapies for acne: a comprehensive update for dermatologists. Dermatol Ther (Heidelb). 2025;15:45-59. doi:10.1007/s13555-024-01324-8, https://pubmed.ncbi.nlm.nih.gov/39751745/
- Perché P, Peck G, Robinson L, et al. Prescribing trends for acne vulgaris visits in the United States. Antibiotics. 2023;12(2):269. doi:10.3390/antibiotics12020269, https://pubmed.ncbi.nlm.nih.gov/36830180/
- Lucky AW. Quantitative documentation of a premenstrual flare of facial acne in adult women. Arch Dermatol. 2004;140(4):423-424. doi:10.1001/archderm.140.4.423, https://pubmed.ncbi.nlm.nih.gov/15096370/















