Gestational diabetes mellitus (GDM) is a type of diabetes that develops during pregnancy when the body is not able to use insulin effectively. This leads to higher-than-normal blood sugar levels during pregnancy.
During pregnancy, the placenta produces hormones that support your baby’s growth. However, these hormones can interfere with insulin function. As a result:
- Glucose stays in the blood instead of entering the cells
- This leads to high sugar levels during pregnancy
- This condition is called insulin resistance
Unlike type 1 diabetes, gestational diabetes is not caused by a lack of insulin. Instead, it happens because pregnancy hormones make insulin less effective.
In most cases, gestational diabetes symptoms improve after delivery, but it is still important to monitor your health after pregnancy.
Globally, gestational diabetes affects many pregnancies. Studies suggest that around 3 to 8 percent of pregnant women may develop this condition, though this number can be higher in some populations, including India.
Key takeaways
- Gestational diabetes is common and manageable
- It is caused by hormonal changes during pregnancy
- Regular monitoring is essential
- Diet and lifestyle play a key role
- Most women have healthy outcomes with proper care
What is the pathology of gestational diabetes mellitus?
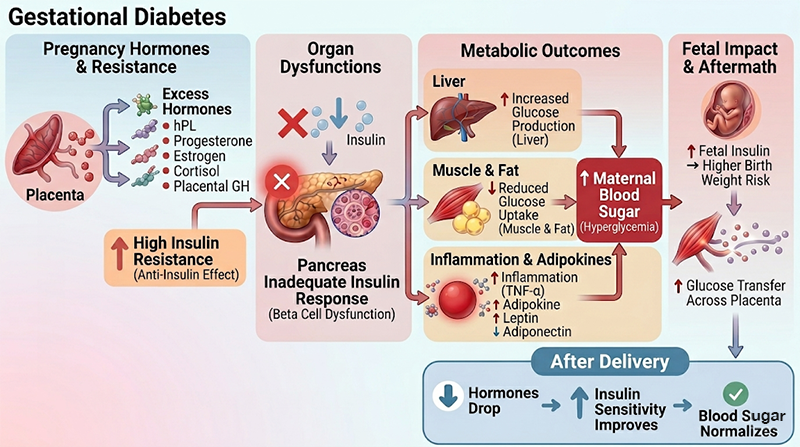
The pathology of gestational diabetes mellitus (GDM) is primarily driven by increased insulin resistance combined with an inadequate response from the pancreatic beta cells during pregnancy. As pregnancy progresses, especially in the second and third trimesters, the body naturally becomes more insulin resistant to ensure a steady supply of glucose to the growing fetus. This process is influenced by placental hormones such as human placental lactogen, progesterone, estrogen, cortisol, and placental growth hormone, which act as anti-insulin factors and reduce insulin sensitivity in tissues like muscle and fat. As a result, glucose uptake by these tissues decreases, leading to higher levels of glucose in the bloodstream.
In a healthy pregnancy, the pancreas compensates by increasing insulin secretion. However, in women with gestational diabetes, the pancreatic beta cells are unable to produce enough insulin to overcome this resistance. This inadequate compensation may be linked to underlying factors such as genetic predisposition or pre-existing insulin resistance.. Additionally, the liver continues to produce glucose through gluconeogenesis, and due to reduced insulin effectiveness, this production is not adequately suppressed, contributing further to elevated fasting blood sugar levels.
There are also changes in inflammatory markers and adipokines, such as increased tumour necrosis factor alpha and altered levels of leptin and adiponectin, which further worsen insulin resistance. Altogether, these mechanisms lead to maternal hyperglycemia, which allows more glucose to cross the placenta, increasing the risk of fetal hyperinsulinemia and excessive fetal growth. After delivery, when placental hormone levels rapidly decline, insulin sensitivity improves, and blood sugar levels usually return to normal. However, gestational diabetes reflects an underlying metabolic vulnerability, which is why affected women have a higher long-term risk of developing type 2 diabetes.
What causes gestational diabetes mellitus?
The exact cause of gestational diabetes mellitus is not fully known, but it is mainly linked to hormonal changes during pregnancy.
Here is what happens in a simple way:
- The placenta produces hormones such as estrogen, cortisol, and human placental lactogen
- These hormones help your baby grow but can block insulin action
- This is called the contra-insulin effect
- It usually begins around 20 to 24 weeks of gestation
As pregnancy progresses:
- The placenta grows larger
- Hormone levels increase
- Insulin resistance becomes stronger
Normally, the pancreas produces extra insulin to balance this effect. But if the body cannot produce enough insulin, gestational diabetes develops.
What are the early symptoms of gestational diabetes?
Gestational diabetes symptoms are often mild or not noticeable.
Some women may experience:
- Increased thirst
- Frequent urination
- Fatigue
- Blurred vision
What are the risk factors for gestational diabetes?
Understanding risk factors for gestational diabetes can help you stay aware.
Common risk factors include:
- Being overweight or obese
- Family history of diabetes
- Age above 25 years
- Previous baby with high birth weight
- History of gestational diabetes in earlier pregnancy
- Prediabetes or impaired glucose tolerance.
It is important to remember that even women without risk factors can develop this condition.
How is gestational diabetes diagnosed?
Doctors usually screen for gestational diabetes between 24 to 28 weeks of pregnancy.
Tests include:
- Glucose Challenge Test
- Oral Glucose Tolerance Test (OGTT)
Women with risk factors may be tested earlier. After delivery, follow-up testing is recommended within 6 to 12 weeks, and regular screening every few years.
What are the risks of high blood sugar during pregnancy?
If sugar level during pregnancy is not well managed, it may affect both mother and baby.
For the baby:
- Larger than normal size
- Early birth
- Breathing problems
- Low blood sugar after birth
- Rare risk of stillbirth
For the mother:
- Higher chance of caesarean delivery
- Increased risk of type 2 diabetes later
The reassuring part is that proper care can greatly reduce these risks.
Normal blood sugar level during pregnancy
Understanding the normal sugar level in pregnancy is very important.
Normal sugar level in pregnancy: 1st, 2nd and 3rd trimesters
| Trimester | Fasting (mg/dL) | 1 Hour Post Meal | 2 Hour Post Meal | HbA1c Target |
| 1st Trimester | <92 | <140 | <120 | <6.5% |
| 2nd Trimester | <92 | <140 | <120 | <6.5% |
| 3rd Trimester | <95 | <140 | <120 | <6.5% |
- Fasting: below 92 mg/dL
- 1 hour after meal: below 140 mg/dL
- 2 hours after meal: below 120 mg/dL
| Sugar Level | When Measured | Meaning | Action |
| Below 92 | Fasting | Normal | Continue monitoring |
| 92-125 | Fasting | Gestational diabetes range | Lifestyle changes |
| 160 | Post meal | High | Consult doctor |
| Above 200 | Anytime | Emergency | Immediate care |
How to manage pregnancy blood sugar levels

The management of gestational diabetes mellitus focuses on keeping blood sugar stable.
How to control sugars in pregnancy
- Eat small, frequent meals
- Choose whole grains and fiber-rich foods
- Avoid refined sugars
How to reduce sugar level during pregnancy naturally
- Daily walking
- Staying hydrated
- Managing stress
How to lower blood sugar during pregnancy without medication
- Timely meals
- Balanced nutrition
- Regular monitoring
Some women may need insulin based on a doctor’s advice.
Pregnancy diabetes diet: what to eat and what to avoid
Diet plays a very important role in managing gestational diabetes and maintaining healthy blood sugar levels during pregnancy. The goal is not to restrict food completely, but to create a balanced and steady pattern that supports both you and your baby.
What to eat when you have gestational diabetes
Choosing the right foods can help keep your sugar levels stable throughout the day.
Include more of these:
- Whole grains like brown rice, oats, and whole wheat
- High fiber foods such as vegetables, lentils, and beans
- Lean proteins like eggs, paneer, tofu, chicken, and fish
- Healthy fats from nuts, seeds, and small amounts of ghee or oil
- Low-glycemic index fruits in controlled portions
- Plenty of water to stay hydrated
These foods help slow down sugar absorption and prevent sudden spikes in glucose levels.
Fruits to avoid during pregnancy with diabetes
Some fruits can raise blood sugar levels quickly, so it is better to limit or carefully portion them.
| Fruits to Limit | Better Alternatives (low glycemic index fruits) |
| Mango | Jamun (blackberry) |
| Banana | Guava |
| Grapes | Apple (with skin) |
| Chikoo (sapota) | Pear |
| Dates | Strawberry |
You do not need to avoid fruits completely. Instead, choose low glycemic index fruits and eat them in small portions, preferably between meals.
What to avoid in diabetes during pregnancy
Certain foods can cause rapid spikes in sugar level during pregnancy and should be limited.
- Sugary drinks like sodas, packaged juices, and sweetened beverages
- Processed foods such as chips, biscuits, and fast food
- Refined carbohydrates like white bread, white rice, and bakery items
- Large portion sizes, even of healthy foods
Guidance for daily eating
- Eat small, frequent meals every 2 to 3 hours
- Do not skip meals, especially breakfast
- Combine carbohydrates with protein for better balance
- Monitor how your body responds to different foods
Track your pregnancy and glucose levels with ease
If you are pregnant, staying aware of your health can feel like a lot. Tracking your blood sugar levels during pregnancy and your baby’s growth can help you feel more in control and supported.
With the Premom App, you can:
- Track your pregnancy week by week
- Monitor your glucose levels in one place
- Get simple insights about your baby’s development
- Set reminders for doctor visits and follow ups
Keeping everything in one place makes it easier for your healthcare provider to review your progress and guide you better.
Regular follow ups are very important in pregnancy, and having your data organized can help you feel more confident at every step of your journey.
Frequently asked questions about gestational diabetes
It is a condition where blood sugar rises during pregnancy.
Fasting sugar above 95-100 mg/dL may indicate gestational diabetes.
Yes, it usually resolves after delivery.
Uncontrolled diabetes may increase risk, but proper care reduces it significantly.
Disclaimer: This article is for informational purposes only and is not a substitute for medical advice, diagnosis, or treatment. Always consult your healthcare provider for personalized guidance.
References
- National Institute of Diabetes and Digestive and Kidney Diseases. Gestational diabetes. U.S. Department of Health and Human Services. https://www.niddk.nih.gov/health-information/diabetes/overview/what-is-diabetes/gestational. Accessed April 17, 2026.
- World Health Organization. Diabetes in pregnancy. https://www.who.int/health-topics/diabetes. Accessed April 17, 2026.
- MedlinePlus. Gestational diabetes. https://medlineplus.gov/gestationaldiabetes.html. Accessed April 17, 2026.



